CASE
REPORT
–
OPEN
ACCESS
InternationalJournalofSurgeryCaseReports46(2018)31–33
Contents lists available atScienceDirect
International
Journal
of
Surgery
Case
Reports
j o u r n a l h o m e p a g e :w w w . c a s e r e p o r t s . c o m
Breast
cancer
cutaneous
metastases
mimicking
Papilloma
Cutis
Lymphostatica.
Biopsy
to
avoid
pitfalls
Giuseppe
Giudice,
Michelangelo
Vestita,
Fabio
Robusto,
Paolo
Annoscia,
Francesco
Ciancio
∗,
Eleonora
Nacchiero
DepartmentofPlasticandReconstructiveSurgery,UniversityofBari,Italy
a
r
t
i
c
l
e
i
n
f
o
Articlehistory: Received8January2018 Accepted19March2018 Availableonline10April2018
Keywords: Breastcancer Lymphedema
PapillomaCutisLymphostatica Metastases
a
b
s
t
r
a
c
t
INTRODUCTION:Secondarylymphedemaisthemostfrequentlong-termcomplicationofaxillary lym-phadenectomy.Itcanresultincomplicationaserysipelas,warts,PapillomaCutisLymphostatica(PCL),or angiosarcomas.Moreover,inwomenaffectedbybreastcanceranaccuratedifferentialdiagnosisamong theseconditionsorcomplicationrelatedtoradiationdermatitisorcutaneousmetastasisisessential. PRESENTATIONOFCASE:Wereportthecaseofa60-year-oldpostmenopausalCaucasianwomanaffected bysecondarylymphedemafollowingcompletemastectomyforbreastcancer.Thepatientaftersurgery wastreatedwithradiotherapy,chemotherapyandhormonetherapy,developingalympedemaofleft armafterfewmonths.TheselesionshadclinicaltypicalfeaturesofPCL,buthistopathologicalanalysis revealeddermo-hypodermicmetastasisofbreastcarcinoma.
DISCUSSION:Thepresenceofskinlesionsinsecondarylymphedemaafteroncologicallymphadenectomy requiresanaccuratedifferentialdiagnosis.Infact,theselesionscanemulatedegenerativeorinfective skindiseases;anyway,inpatientsaffectedbysecondarylymphedemaotherlesscommonconditions– asPLC,nodular-typelichenmyxedematosusorGottron’scarcinoidpapillomatosis–shouldbetakeninto account.
CONCLUSION:Ourcasereportsthepossibilitythatmetastasesofbreastcancermightalsomimicthese conditions.
©2018TheAuthor(s).PublishedbyElsevierLtdonbehalfofIJSPublishingGroupLtd.Thisisanopen accessarticleundertheCCBY-NC-NDlicense(http://creativecommons.org/licenses/by-nc-nd/4.0/).
1. Introduction
Secondarylymphedema ofupper limbsisthemostfrequent long-term complication of axillary lymphatic tissue resections, withanincidencerangingbetween6%and30%[1].Mostfrequent sequelaoflymphedemaareerysipelasandwarts,butinveryrare casesit canresultin moreseverecomplications, suchas Papil-lomatosisCutis Lymphostatica(PCL)or angiosarcomas.PCLis a benign,usuallyasymptomaticandunderreportedcondition result-ingfromchroniclymphedema[2].Itwasmorefrequentlyreported inprimarylymphedemaorascomplicationofasecondary dam-ageoflymphaticvesselsduetodiabetes.Todate,fewcasesofPCL havebeendocumentedafteraiatrogenicsecondarylymphedema [3,4].Alsocarcinomasorangiosarcomasarisinginlimbsaffected bychroniclymphedemahavebeendocumented[5,6].Moreover, lesionsarisingin upper limbin women affectedby breast car-cinoma could be related to cutaneous metastases or radiation dermatitisfollowingradiationtherapy[7,8].Forthis reason,the
∗ Correspondingauthorat:DepartmentofPlasticandReconstructiveSurgery, UniversityofBari,CAP70124PiazzaGiulioCesare11,Bari,Italy.
E-mailaddress:[email protected](F.Ciancio).
presence ofskinlesionsoftheupperlimbsin patientsaffected bybreastcancerrequiresanaccuratedifferentialdiagnosisamong cancerrecurrencesormetastasis,therapeuticalcomplications,and dermatologicalconditions.Theworkhasbeenreportedinlinewith theSCAREcriteria[9].
2. Casereport
Wepresentthecaseofa60-year-oldpostmenopausalCaucasian woman affectedbysecondary lymphedema following complete mastectomyandaxillarydissectionforaLuminalBinvasivelobular carcinomaofleftbreast.Immunohistochemistrytestifiesnegativity forHER-2mutation.Patientunderwentmastectomyandcomplete lymphadenectomyofleftaxillaryregioninNovember2015.The patientrefusedthereconstructivesurgicaltreatmentofthebreast. After surgery, the case was presented to the multidisciplinary breastcancerboardofourinstitutionandthepatientunderwent localradiotherapyandadjuvantchemotherapybasedon anthracy-cline/taxaneregimenfollowedbyhormonetherapywithletrozole. InOctober2016,thepatientpresentedwithastageIIIleftupper limblymphedema[10]withtheappearanceofisochromicnodular lesionsoftheskin(Figs.1and2).Segmentallymphoscintigraphy ofupperlimbsdocumentedaseverelymphedemaoftheleftupper
https://doi.org/10.1016/j.ijscr.2018.03.025
2210-2612/©2018TheAuthor(s).PublishedbyElsevierLtdonbehalfofIJSPublishingGroupLtd.ThisisanopenaccessarticleundertheCCBY-NC-NDlicense(http://
CASE
REPORT
–
OPEN
ACCESS
32 G.Giudiceetal./InternationalJournalofSurgeryCaseReports46(2018)31–33
Fig.1.Initialclinicalpresentationoflesions.
Fig.2. Detailofinitialnodularlesion.
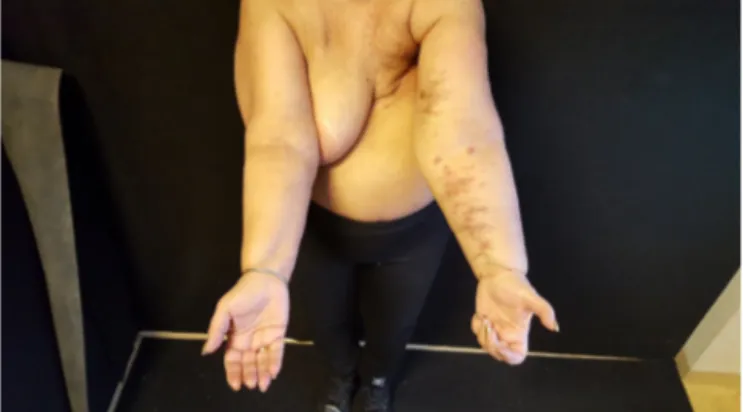
Fig.3. Clinicalpresentationofmultiplenodularreddenedlesions.
limbwithahighvalueofTransportIndex(28),while lymphoscinti-graficexaminationwasnormal in thecontralateral upperlimb. Thepatientunderwenttherapywithphysiotherapy,bandagesand plasticdevices;inDecember2016,however,thepatientreported furtherdiffusionandreddeningof theskinlesionsaffectingthe leftupperlimb(Figs.3and4).Thephysicalexaminationrevealed thepresenceofpainlessnon-confluentovalnodularlesions, dis-tributedonthevolarsurfaceofleftarmand forearm.Clinically, theselesionshadthetypicalfeaturesoflymphostatic papillomato-sis;nonetheless, due tothepatient’s history, we performedan excisionalbiopsyofone ofthelesions.Histopathologicanalysis revealedthepresenceof0.7cm masscharacterizedbypresence ofpleomorphicspindlecellswithlargehyper-chromaticnucleiand denseeosinophiliccytoplasm.Immunohistochemistrywaspositive forproteinKi67andestrogenreceptor,confirmingthediagnosisof dermo-hypodermicmetastasisofinvasivebreastcarcinoma.The patientwasconsideredhormone-refractory and sheunderwent tofirstlinechemotherapywithanti-VEGFincombinationto
tax-Fig.4.Detailofreddenedlesions.
ane.Todate,shehasundergoneclinicalandimaging(chestX-ray, abdominalultrasound,andwhole-bodySPECT/CTscan)follow-up withnoevidenceoflymphaticorvisceralmetastases.
3. Discussion
Presenceofovalexophiticnon-pigmentedlesioninthe homo-lateralupper limb of womanwho underwent mastectomy and completelymphadenectomyofaxillaryregionforabreastcancer needanaccuratedifferentialdiagnosis,evenmoreinpresenceof lymphedema.
First of all,differential diagnosis includes degenerative skin conditions such as keratoacanthoma, pilomatricoma, pyoderma vegetans, and non-pigmented skin cancers; however the pres-enceofmultipleexophiticlesionsmakestheseunlikelydiagnoses. Infectivecomplicationsoflymphedemaaremoreplausibleinthis patient;infact,lymphedemaisthemostcommonlong-term com-plicationofaxillarylymphnodedissection[1]andassociationof reducedimmunesurveillanceandskindamageinthe lymphede-matousregions[11]mayleadtoskininfections.Inmoresevere cases,lymphedemacanresultinpapillomatosiscutis lymphostat-ica(PCL),characterizedbythepresenceofmultipleskin-colored, confluent,partlyhyperkeratotic,verrucouspapulesonlimbs[6].In suchcases,skininfections,aserysipelas,mayresultfromskinlossof continuity.Wartsandangiosarcomaswerealsoreportedinpatients affectedbyPCL[5,6]. Finally,nodular-type lichen myxedemato-susandGottron’s carcinoidpapillomatosis[12]skinshouldalso beconsideredincaseofmultipleexophyticlesionsonlimbs,but theabsenceofhypothyroidismandthenegativityforHPVserology assayexcludethesediagnoses.
Alloftheaboveconditionsarecompatibleswiththeskinlesions affectingtheleftupperlimbofourpatient;cutaneousmetastasesof breastcancer,ontheotherhand,havebeendocumentedinseveral studies,asevidencedbyourresearchatoneofthemost impor-tantdatabasesintheliterature[13].Thesecanbepolymorphous, mimickingwhealrash[14],erythemaannullarecentrifugum[15], nodules[16]orexophyticlesions[7].
Inanycase,excisionalbiopsyisindispensableforacorrectand precociousdiagnosisofskinmetastasisofbreastcancermimicking PCLinalimbaffectedbylymphedema.Furthermore,asinourcase, skinmetastasesmaybethefirstclinicalevidenceofrecurrenceand theirdetectionimpliestheadjustmentofchemotherapyregimen andthusholdsprognosticandtherapeuticsignificance.
Conflictsofinterest
CASE
REPORT
–
OPEN
ACCESS
G.Giudiceetal./InternationalJournalofSurgeryCaseReports46(2018)31–33 33
Funding
Authorshavenotreceivedfundingorsponsorforpaper produc-tion.
Ethicalapproval
Tocarryoutthisscientificwork,therewasnoneedtoresort totheethicscommittee.Ethicalapprovalhasbeenexemptedfrom ourinstitution.
Consent
Writteninformedconsentwasobtainedfromthepatientfor publicationofthiscasereportandaccompanyingimages.Acopy ofthewrittenconsentisavailableforreviewbytheEditor-in-Chief ofthisjournalonreques.
Authorcontribution
Alltheauthorscontributedequallytothewritingofthepaper. Researchregistrationnumber
NA. Guarantor
FrancescoCiancioMD. References
[1]J.A.Petrek,M.C.Heelan,Incidenceofbreastcarcinoma-relatedlymphedema,
Cancer83(1998)2776–2781.
[2]R.S.Kasper,S.Nobbe,Imagesinclinicalmedicine.Papillomatosiscutis
lymphostatica,N.Engl.J.Med.370(January(1))(2014)69,http://dx.doi.org/
10.1056/NEJMicm1307463.
[3]D.Aydin,M.Heidenheim,Papillomatosiscutislymphostatica,Clin.CaseRep.
4(September(10))(2016)1012(eCollection2016Oct.).
[4]M.Guida,A.Cramarossa,E.Fistola,M.Porcelli,G.Giudice,K.Lubello,G.
Colucci,Highactivityofsequentiallowdosechemo-modulating
TemozolomideincombinationwithFotemustineinmetastaticmelanoma.A
feasibilitystudy,J.Transl.Med.8(November)(2010)115.
[5]H.H.Niederauer,U.Schultz-Ehrenburg,K.U.Tiedjen,Tumorformof
lymphostaticpapillomatosisoftheskin,Hautarzt42(August(8))(1991)
518–522(ArticleinGerman).
[6]J.I.Epstein,G.Mendelsohn,Squamouscarcinomaofthefootarisingin
associationwithlong-standingverrucoushyperplasiainapatientwith
congenitallymphedema,Cancer54(September(5))(1984)943–947.
[7]U.Handa,R.Kundu,K.Dimri,Cutaneousmetastasisastudyof138cases diagnosedbyfine-needleaspirationcytology,ActaCytol.(December)(2016),
http://dx.doi.org/10.1159/000453252.
[8]F.N.Bray,B.J.Simmons,A.H.Wolfson,K.Nouri,Acuteandchroniccutaneouss
reactionstoionizingradiationtherapy,Deematol.Ther.(Heidelb.)6(June(2))
(2016)185–206.
[9]R.A.Agha,A.J.Fowler,A.Saetta,I.Barai,S.Rajmohan,D.P.Rajmohan,The
SCAREGroup,TheSCAREstatement:consensus-basedsurgicalcasereport
guidelines,Int.J.Surg.34(October)(2016)180–186.
[10]InternationalSocietyofLymphology,Thediagnosisandtreatmentof
peripherallymphedema:2013ConsensusDocumentoftheInternational
SocietyofLymphology,Lymphology46(March(1))(2013)1–11.
[11]W.J.Stewart-Treves,Syndrome:alethalcomplicationofpostmastectomy
lymphedemaandregionalimmunedeficiency,Arch.Surg.(1979)11482.
[12]H.H.Niederauer,U.Schultz-Ehrenburg,K.U.Tiedjen,Tumorformof
lymphostaticpapillomatosisoftheskin,Hautarzt42(August(8))(1991)
518–522.
[13]LoRusso,G.Spolveri,F.Ciancio,F.A.Mori,Mendeley:aneasywaytomanage, share,andsynchronizepapersandcitations,Plast.Reconstr.Surg.131(6) (2013)946e–947e,http://dx.doi.org/10.1097/PRS.0b013e31828bd400.
[14]C.Damaskos,D.Dimitroulis,V.Pergialiotis,C.Doula,G.Koulermou,E.A.
Antoniou,M.Frangoulis,K.Stergios,K.Kontzoglou,Anunexpectedmetastasis
ofbreastcancermimickingwhealrush,G.Chir.37(May–June)(2016)
136–138.
[15]V.Sabater,F.Ferrando,A.Morera,L.Palomar,Cutaneousmetastasisof inflammatorybreastcarcinomamimickinganerythemaannulare centrifugum:asignoflocallyrecurrentcancer,Clin.Exp.Dermatol.41 (December(8))(2016)906–910,http://dx.doi.org/10.1111/ced.12953.
[16]S.Kamaraju,J.Depke,J.Povletich,A.Currey,E.Weil,Cutaneousmetastasis
duetoBreastcancerinapatientwithprimarybiliarycirrhosis:acasereport,
CaseRep.Oncol.9(November(3))(2016)718–725.
OpenAccess
ThisarticleispublishedOpenAccessatsciencedirect.com.ItisdistributedundertheIJSCRSupplementaltermsandconditions,which permitsunrestrictednoncommercialuse,distribution,andreproductioninanymedium,providedtheoriginalauthorsandsourceare credited.