CASE
REPORT
–
OPEN
ACCESS
InternationalJournalofSurgeryCaseReports16(2015)134–136ContentslistsavailableatScienceDirect
International
Journal
of
Surgery
Case
Reports
jo u r n al ho me p a g e :w w w . c a s e r e p o r t s . c o m
Refractory
hepatic
lymphorrhea
after
total
pancreatectomy.
Case
report
and
literature
review
of
this
uncommon
complication
Michele
Bartoli
∗,
Gian
Luca
Baiocchi,
Nazario
Portolani,
Stefano
Maria
Giulini
DepartmentofMedicalandSurgicalSciences,SurgicalClinic,UniversityofBrescia,BresciaCivilHospital,P.leSpedaliCivili,1,25123Brescia,Italy
a
r
t
i
c
l
e
i
n
f
o
Articlehistory:
Received20August2015 Receivedinrevisedform 14September2015 Accepted18September2015 Availableonline26September2015 Keywords:
Refractoryhepaticlymphorrhea Chylousascites
Lymphadenectomy Hepatoduodenalligament Lymphangiography
a
b
s
t
r
a
c
t
INTRODUCTION:Afterextendedabdominallymphoadenectomy,lymphaticvesselinjurymaycause lym-phorrhea thatusuallydisappears spontaneously.However, intractableascitessometimes develops. Althoughtherearemanyreportsdescribingpersistentchylousascitesfromintestinallymphorrhea,little isknownabouthepaticlymphorrhea,notcontainingchyle.Itiscausedbyinjuryofthelymphaticvessels duringhepatoduodenalligamentlymphadenectomy.
Wepresentacaseofmassiveascitesduetohepaticlymphorrheaaftertotalpancreatectomyand extendedlymhoadenectomyforAmpullaradenocarcinoma.Wesuccessfullytreateditwithprolonged medicaltherapyaftersurgicalrelaparotomy.
PRESENTATIONOFCASE:A65-yearoldmanunderwenttotalpancreatectomywithextendednodal dis-section.Massiveclear-coloredascites(2000–9000mLperday)developedsincethesecondpostoperative dayandpersisteddespiteconservativetherapy.Atre-laparotomynolymphaticleakagewasfound. Sim-ilarlylymphangiographywasshowednocontrastspreading.Wetreatedthishepaticlymphorreawith intermittentopeningoftheabdominaldrainageuntilspontaneousresolution.
DISCUSSION:Thestandardtreatmentofhepaticlymphorrheaisanaggressivemedicaltreatment.After suchapproachthemosteffectivetherapyseemstobesurgicalexploration.Otheroptionare peritoneove-nousshuntorintraperitonealadministrationofOK-432.
CONCLUSION:Inourexperiencetheintermittentabdominaldrainageuntilspontaneousresolutionisan usefulapproachtohepaticlymphorrhea.
©2015TheAuthors.PublishedbyElsevierLtd.onbehalfofSurgicalAssociatesLtd.Thisisanopen accessarticleundertheCCBY-NC-NDlicense(http://creativecommons.org/licenses/by-nc-nd/4.0/).
1. Introduction
Duringabdominalsurgery,especiallyafterextended lymphoad-enectomyforgastricorpancreaticcancer,lymphaticvesselinjury causeslymphorrhea.Thepostoperativelymphorrheausually dis-appearsspontaneouslyinafewdays.However,intractableascites may develop especially in patients with liver cirrohosis, heart failureorrenalfailure.Althoughtherearemanyreports describ-ing the diagnosis, causes and treatment of persistent chylous ascites fromintestinallymphorrhea, littleis knownabout hep-atic lymphorrheafollowing abdominal surgery. It is caused by injuryofthelymphaticvesselsespeciallyduringthe hepatoduo-denalligmanetlymphadenectomy.Usuallyconventionalmedical treatmentssuchascessationoforalintake,totalparenteral nutri-tion,diuretictherapy,albuminsupport,intravenousreinfusionof ascites,ortherapeuticparacentesisareunsuccessful.Wepresent acaseofintractablemassiveascitesduetohepaticlymphorrhea aftertotal pancreatectomyand extended lymhoadenectomy for
∗ Correspondingauthor.
E-mailaddress:[email protected](M.Bartoli).
Ampullaradenocarcinoma,successfullytreatedwithconservative approachafterineffectivesurgicalrelaparotomy.
2. Presentationofcase
A65-yearoldmanwashospitalizedduetoobstructivejaundice. AnadenocarcinomaofVaterpapillawithnodalinvolvementwas diagnosedbyabdominalTCscanandERCP.Preoperativestaging wasT2N+.ASAgradewas3.Intra-operativefindingofsoft pan-creasandlittleWirsungduct(<3mm)promptedustoperformtotal pancreatectomy.Suspectednodalinvolvementtillinteraortocaval nodeswasfound,soextendedlymphnodedissectionwascarried out(overD2).PostoperativestagingwasT3N1withinvolvementof 2of27nodes.Massiveascites,rangingfrom2000to9000mLper day,developedsincethesecondpostoperativeday.Theasciteswas unresponsivetoalbuminandelectrolytesupport,administration ofmaximaldiureticsdose,diet,totalparenteral nutrition(TPN), continuousdrainage,andoctreotideinfusion.Cytological examina-tionrevealednomalignatcells,andculturewasinitiallynegative. Theascites wasclear-coloredand wasdiagnosedbiochemically asnonchylouslymphorrheawithtotal proteinconcentrationof 3g/dL,albuminconcentration1,5g/dLandserum-ascitesgradient http://dx.doi.org/10.1016/j.ijscr.2015.09.023
2210-2612/©2015TheAuthors.PublishedbyElsevierLtd.onbehalfofSurgicalAssociatesLtd.ThisisanopenaccessarticleundertheCCBY-NC-NDlicense(http:// creativecommons.org/licenses/by-nc-nd/4.0/).
CASE
REPORT
–
OPEN
ACCESS
M.Bartolietal./InternationalJournalofSurgeryCaseReports16(2015)134–136 135
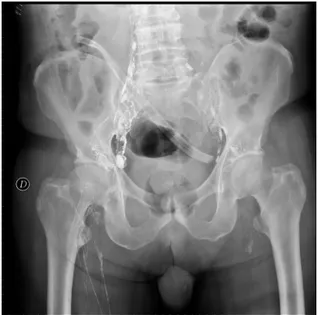
Fig.1. Lymphangiographyshowingnocontrastspreading.
1g/dL.Themainconstituentoftheasciteswashepaticlymph.It derivedfromsurgicalinjuryofthelymphaticsinthe hepatoduo-denalligament.Inthe19thpostoperativeday(POD)wedecided toperformsurgicalre-exploration.Howevernoobviouslymphatic leakagepointwasfoundevenafteradministrationoffattymeal throughnaso-gastrictubeandLipofundin(BBraun; Melsungen; Germany)injectioninlymphaticvessels.Meticulousexplorationof hepatoduodenalligamentwasperformed;eveninabsenceofclear leakage,surgicalligationofinteraortocavaltissuesand Atossis-clerol(ChemischeFabrikKreussler&Co.;Wiesbaden;Germany) application in hepatoduodenal ligament were carried out. Also Tachosil(Takeda; Linz;Austria) wasappliedtotreat lymphatic leakages.
Aftersurgicaltreatmenttherewasnochangein theamount of the drainage (about 4000–9000mL/day). The patient’s daily activitiesworsened,duetodisturbanceofmobilityandfever com-promisingrespiratoryfunctiontillacuterespiratoryfailure.
Inthe34thPOD,duetotheincreasingoflymphorrhea, lym-phangiographywasperformedinanattempttoidentify(andtreat withlymphaticembolization)anunrecognizedleakage.However nocontrastspreadingwasfound(Fig.1).
The patient developed sepsis sustained by Pseudomonas Aeruginosaatfirst,andthenbymulti-resistentKlebsiella Pneu-moniae and Candida Albicans. He also suffered from septic chorioretinitis that required surgical treatment (vitrectomy) in additiontotargetedantibiotictherapy.
The postoperative course was characterized by progressive weightloss,hypoalbuminemia,electrolyteimbalanceanddiffuse edema. We decided toclose theabdominal drainage for a few days.Thisoption caused asthenia,appetite loss,nausea, vomit-ing,fullnesssensation,abdominaldistention,peripheraledemaand requiredparenteralsupportandcarefulenteralnutritionwithnose gastrictube.
Theintermittentopeningofthedrainage,causedthe progres-sivedecreaseofthelymphorrhea.After132dayswecouldremove thetube. The patient wasdischarged in the 181th POD.At 12 monthsfollow-up,thepatientisalive,diseasefree andhasfair generalconditionswithoutlymphorrhearecurrence.
3. Discussion
Intraabdominallymphpathwaysaremanlyclassifiedinto hep-aticandintestinal.both Thesepathwaysdrainintothecisterna
chyliand subsequently intothecirculatorysystemthrough the thoracicduct.Thehepaticlymphaticsystemhastwomajor path-ways(ascendinganddescending)ofdrainage.Viatheascending pathways,lymphfromthesurfaceoftheupperpartoftheliver flows along thediaphragm intothecisterna chyli whilelymph fromtheliverbedandintheliverflowsalongthehepaticveins. Thedescendingpathwayrunsthroughthehepatoduodenal liga-mentwithportalvein,hepaticarteryandbileduct.Intestinallymph drains50–75%ofintraabdominallymphandcontainsmainlylipid dropletsoflongchainfattyacids;thusitscolorismilky.Ontheother hand,hepaticlymphdrains25–50%ofintraabdominallymph.This lymphcontainsproteinsofthesamedensityasplasmawithout lipiddropletsandisclear-colored[1,2].
Intra abdominal lymphorrhea, without chylous ascites, is a rarecomplicationafterabdominalsurgery.Itresultsfrominjury ofthelymphaticvesselsparticularlyinthehepatoduodenal liga-ment.Althoughsmalllymphleaksarecommonlyleftopenduring lymphadenectomy,theyrarelycauselymphorrheabecauseofthe abundanceofcollaterallymphaticchannelsandtheregeneration ex-novo oflymphatics. Therefore theyusually remainclinically asymptomaticorunrecognized.Lymphorreabecomesintractable incases ofinjurytomajorlymphaticvesselsand when repara-tivemechanismsbecomeinsufficient. Littleis knownaboutthe managementofpostoperativehepaticlymphorrea.Toour knowl-edge,thereisonlyonereportofhepatic lymphorrheafollowing abdominalsurgeryintheWesternmedicalliterature[3],andless thantwentycasesinEasternmedicalliterature[4].After diagno-sisofpostoperativehepaticlymphorrhea,allpatientsweretreated conventionallybydiet,TPN,diureticsandtherapeuticparacentesis. We performed an aggressive medical treatment since the presentation of lymphorrhea by TPN, massive diuretics ther-apy,continuous drainage, albuminand electrolyte supportand octreotideinfusion.Themechanismby whichoctreotideaffects lymphorreaisunknown.Ithasalsobeenspeculatedthat somato-statininhibits lymph fluid excretion through specific receptors foundinthenormallymphaticvessels.
After conventional medical treatment, various regimens are usedtotreattheintractablehepaticlymphorrhea(Table1).The mosteffective therapyappears tobesurgicalligationoflymph fistulawithsclerotherapyand/orfibringluesprinkleevenifthe pre-operativeimagingstudydoesnotshowanobviousleakagepoint
[4].
Wecarriedoutsurgicalligationearlierthanotherauthors,even inabsenceofobviousleakagepoint,becauseofamountof lymphor-reaandresistancetoallconservativetherapies.Noauthorreported ascites more than4500mLper day.Atthe time ofreoperation thepatientsbotheredlymphorrhearangingfrom4000to8000mL perday,drainedbytheabdominaldrainagetube.Itcausedsevere andpotentiallylife-threateningipokalimia,albumindepletionand dehydrationdespitemedicaltherapy.
Inoue[5]reportedtheuseofperitoneovenousshunt(PVS)for intractableascitesduetohepaticlymphorrhea.Theplacementof aPVSismainlyusedforintractableascitesduetodecompensated livercirrhosisandforrefractorychylousascites.Itisasimpleand cost-effective procedureeven ifit is linkedtohighmorbidities suchasobstruction,vascularthrombosis,infections,sepsisand dis-seminatedintravascularcoagulopathy.Henceithasbecomealess commontechnique.Moreoverourpatientshowedsignsofsepsis (leukocytosis, fever,highPCR andprocalcytonine value) associ-atedwithP.AeruginosaandKlebsiellapneumoniacolonizationof theascites.ThisconditionhighlycontraindicatedPVSplacement.
Fewauthors[4,6]reportedeffectivetreatmentofhepatic lym-phorrhea using local intraperitoneal administration of OK-432 whichisaheatandpenicillin-treatedpreparationofstreptococcus pyogenes A3. It is largely used in the treatment of lymphat-ics malformations and for malignant ascites. OK-432 promotes
CASE
REPORT
–
OPEN
ACCESS
136 M.Bartolietal./InternationalJournalofSurgeryCaseReports16(2015)134–136Table1
Chracteristics,therapiesandclinicaloutcomeofthepatientswithhepaticlymphorrhea.
Case Author Age/sex Operation Treatment Timetocompleteresolution
1 Miyagawa,1983 65/M TG Surgicalligation 13
2 Nakashima,1985 58/M DG Surgicalligation+sclerotherapy 30
3 Nakano,1987 49/M TG Surgicalligation 14
4 Kawata,1989 52/M DG Surgicalligation+fibringlue+sclerotherapy 37
5 Umehara,1989 59/M TG Surgicalligation 28
6 Kaneko,1991 44/M DG Surgicalligation+PVS 30
7 Imai,1992 34/M TG Reoperation+sclerotherapy 7
8 Shimizu,1992 62/M DG Surgicalligation 30
9 Ota,1993 70/M DG Surgicalligation+fibringlue 50
10 Mitsuno,1993 42/M DG PVS ND
11 Kawahira,1994 58/M DG Surgicalligation+fibringlue+OK-432sclerotherapy 10 12 Matsumoto,1995 44/M DG Re-re-surgicalligation+fibringlue 14 13 Tanaka,1998 49/M DG Surgicalligation+fibringlue+OK-432sclerotherapy 12 14 Tanaka,2004 66/M TG Surgicalligation+fibringlue+OK-432sclerotherapy 67
15 Inoue,2011 73/M HR PVS 12
TG:totalgastrectomy;DG:distalgastrectomy;PVS:peritoneovenousshunt;HR:hepaticresectionND:notdescribed.
reabsorptionofasciticfluidincreasingcapillarypermeabilityand inducing local inflammatory action which causes occlusion of injuredlymphatics.We havenoexperienceofthis kindof scle-rotherapyandtheethicsCommitteedidn’tauthorizetheuseofthis kindofdrugs.
Ourstrategywastoopenandcloseintermittentlytheabdominal drainage.Atfirstthisoptioncauseddiscomforttothepatientbut allowedagradualreductionofspontaneouslymphorrheauntilits resolution.
4. Conclusion
Inourexperience,thisapproachincreasesintraabdominal pres-sureand promotes trans-peritoneal reabsorption. This solution maybeusefulwhen theotheroptions mentioned byliterature provetobeineffectiveorcontraindicated.
Conflictofinterest None. Funding None. Ethicalapproval Notneeded. Consent
Writteninformconsentwasobtainedfromthepatientfor pub-licationsofthiscasereportandaccompanyingimages.Acopyof thewrittenconsentisavailableforreviewbytheEditor-in-Chiefof thisjournalonrequest.
Authorcontribution
MicheleBartoli wastheprincipalinvestigator andwrotethe paper.StefanoMariaGiulini,NazarioPortolaniandGianLuca Baioc-chitreatedthepatient.Allauthorscriticallyreviewedthepaperand approvedthefinalversion.
Guarantor MicheleBartoli. Acknowledgements
None. References
[1]H.Ota,T.Miyazawa,I.Hiizu,etal.,Acasereportofintractableascitesdueto hepaticlymphorrheafromhepatoduodenalligamentafterradicalgastrectomy forgastriccancer,Jpn.J.Gastroenterol.Surg.26(1993)1115–1119.
[2]Y.Kawahira,K.Nakao,M.Nakahara,etal.,Acaseofintractablehepatic lymphorrheaaftergastrectomyforgastriccancer,Jpn.J.Gastroenterol.Surg.27 (1994)117–120.
[3]D.Guez,B.S.Gregory,J.Nadolski,etal.,Transhepaticlymphaticembolizationof intractablehepaticlymphorrhea,J.Vasc.Interv.Radiol.25(1)(2014)149–150.
[4]K.Tanaka,Y.Ohmori,Y.Mohri,etal.,Successfultreatmentofrefractoryhepatic lymphorrheaaftergastrectomyforearlygastriccancer,usingsurgicalligation andsubsequentOK-432(Picibanil)sclerotherapy,GastricCancer7(2004) 117–121.
[5]Y.Inoue,M.Hayashi,F.Hirokawa,etal.,Peritoneovenousshuntforintractable ascitesduetohepaticlymphorrheaafterhepatectomy,WorldJ.Gastrointest. Surg.3(1)(2011)16–20.
[6]Y.Inaba,Y.Arai,K.Matsueda,etal.,Intractablemassiveascitesfollowing radicalgastrectomy,treatmentwithlocalintraperitonealadministrationof OK-432usingaunifiedCTandfluoroscopysystem,Australas.Radiol.47(2003) 465–467.
OpenAccess
ThisarticleispublishedOpenAccessatsciencedirect.com.ItisdistributedundertheIJSCRSupplementaltermsandconditions,which permitsunrestrictednoncommercialuse,distribution,andreproductioninanymedium,providedtheoriginalauthorsandsourceare credited.